Total shoulder replacement surgery is designed to relieve pain and restore mobility, helping patients return to everyday activities with greater comfort. Although outcomes are generally positive, complications can occur, as with any major surgery. In this post, we’ll review the possible complications, what causes them, and the advances in surgical care that help minimize these risks.
Key Takeaways
- Glenoid loosening represents the most common cause of failure following anatomic total shoulder replacement.
- Advancements in shoulder implant technology have been proven to dramatically reduce this problem.
- Selecting an orthopedic surgeon who specializes in shoulder replacement can help prevent problems after shoulder replacement surgery.
Understanding Total Shoulder Replacement
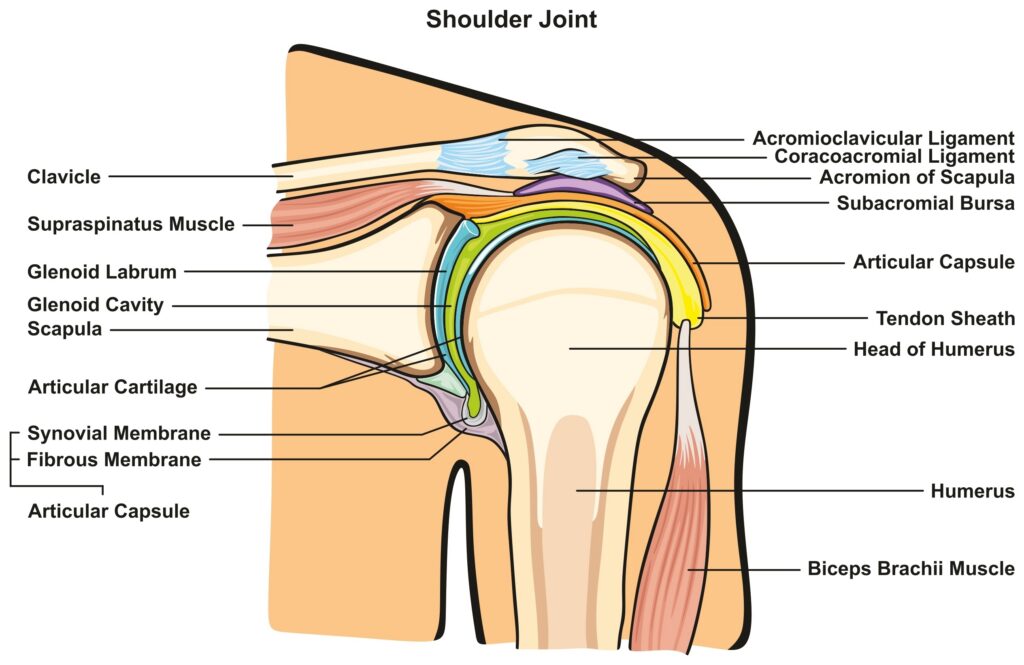
Before discussing potential complications and how they can be prevented, it helps to understand what occurs during total shoulder replacement. Your surgeon removes damaged portions of the shoulder joint and replaces them with artificial components. The humeral head, or ball of the joint, is replaced with a metal implant. The glenoid, which is the socket portion on your shoulder blade, receives a plastic component. This anatomic replacement mimics your natural shoulder structure. When successful, patients frequently experience meaningful pain relief and improved function.
Glenoid Loosening: The Most Common Cause of Failure with Total Shoulder Replacement Surgery
The leading cause of failure with any anatomic total shoulder replacement is glenoid loosening. This occurs when the plastic glenoid component begins to separate from the bone where it was initially secured.
Over time, the forces placed on this component during shoulder movement can create stress at the bone-implant interface. Legacy glenoid implant designs that sit on the bone surface may experience what is called a “rocking horse” motion. This repetitive stress can gradually loosen the component, potentially leading to pain and decreased function years after surgery.
How Glenoid Loosening Progresses
Glenoid loosening is typically not an immediate problem but rather a progressive mechanical failure that develops over months to years. It generally progresses in four stages:
Phase 1: Micromotion
In the early stages, microscopic movement occurs at the interface between the glenoid component and the surrounding bone or cement. You may not feel any symptoms during this phase.
Phase 2: Progressive Bone Loss
As micromotion continues, the gaps widen and extend around more of the component. Bone cells respond to the abnormal movement and stress by resorbing bone around the implant, a process called osteolysis. The cement mantle (if applicable) may develop cracks or defects. At this stage, you might begin to notice:
- Subtle decreases in strength
- Occasional discomfort with certain movements
- A sense that your shoulder isn’t quite as reliable as it was initially
Phase 3: Symptomatic Loosening
When loosening becomes clinically significant, symptoms typically include:
- Pain that develops or returns after a period of good function
- Pain that worsens with activity and may persist at rest
- Decreased range of motion, particularly in external rotation (rotating arm outward) and abduction (lifting arm to the side)
- Grinding, clicking, or clunking sensations
- Weakness and difficulty with daily activities
Phase 4: Component Failure
In advanced cases, the component may:
- Visibly shift position on X-rays
- Tilt or migrate from its original placement
- Develop extensive bone loss around the implant
- Require complex revision surgery with bone grafting
The timeline for this progression varies considerably. Patients who are unfortunate enough to experience glenoid loosening may develop significant loosening within 2-3 years, while others maintain stable glenoid components for 10-15 years or longer.
There are other factors outside of older implant designs that can also contribute to glenoid loosening. Poor bone quality at the time of surgery can affect initial fixation. Implant positioning and alignment also play roles in long-term stability. Additionally, the way forces distribute across the implant surface during shoulder movement can influence how well the component remains secure over time.
How Glenoid Loosening Can Be Prevented
Modern surgical approaches are working to address this challenge. For example, the glenoid technology in the InSet® Shoulder Implant System represents one such advancement. Rather than resting on the surface of the bone, the InSet® glenoid is placed within a pocket of sclerotic bone, which is dense and strong. Hence, the name “In-Set.”
One way to understand this design is to think of a manhole cover. Cars and trucks drive over it every day, yet it remains securely in place. A manhole cover was, in fact, the original inspiration for the surgeon who developed this concept.
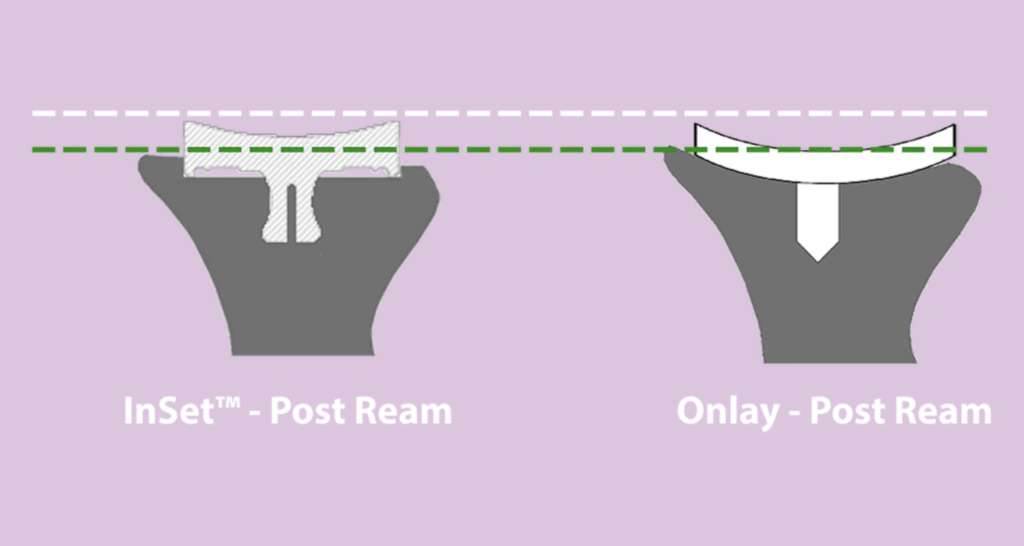
With this design, computer-based mechanical modeling (Finite Element Analysis) has shown up to an 87% reduction in the rocking horse stresses that contribute to loosening. By surrounding the component with a rim of strong bone, the InSet® design:
- Distribute forces more evenly across the component
- Reduce stress concentrations at the implant edge
- Provide mechanical resistance to the tilting motion that causes loosening
- Create a more stable bone-implant interface
This is one of the primary reasons that I use the InSet® system from Shoulder Innovations.
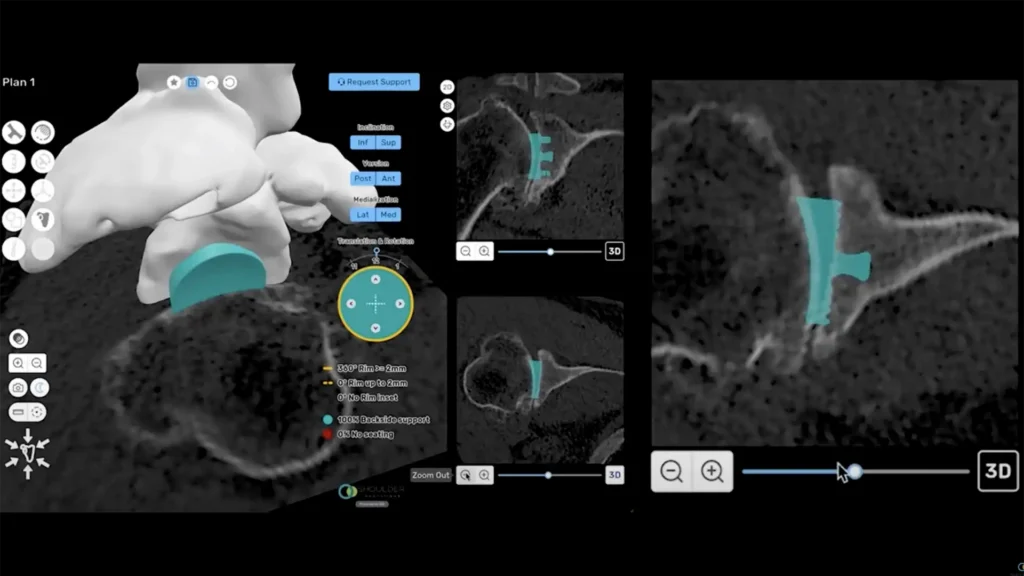
In addition, advanced imaging and pre-operative software planning, such as ProVoyance®, help surgeons plan optimal component positioning based on an individual patient’s anatomy before entering the operating room, further reducing the risk of malpositioning.
Other (Less Common) Problems After Shoulder Replacement Surgery
Infection
Infection following shoulder replacement, while relatively uncommon, represents a complication requiring prompt attention. Infections can occur superficially at the incision or within the joint. Deep infections often necessitate additional surgery to clean the joint and may require temporary or permanent removal of components.
Early signs might include increasing pain, swelling, warmth, redness around the incision, or drainage. Fever can also indicate infection. If you notice these symptoms, contact your surgeon immediately. Early intervention supports better outcomes.
Instability and Dislocation
Shoulder instability after replacement surgery means the ball component can move out of its proper position within the socket. In severe cases, complete dislocation may occur, where the humeral head comes completely out of the glenoid.
Proper component sizing, positioning, and soft tissue balancing during surgery help prevent instability. Your rotator cuff muscles and surrounding shoulder structures also play important roles in maintaining joint stability. If these tissues were significantly damaged before surgery, stability can be more challenging to achieve. An experienced shoulder surgeon who uses preoperative planning software can help improve precision during surgery and potentially reduce these risks.
Symptoms of instability include a feeling that your shoulder might “give out” or slip out of place. Some patients describe a clunking sensation. Recurrent instability may require revision surgery to adjust component positioning or size.
Nerve Injury
Nerves that control shoulder movement and sensation run close to the surgical area. The axillary nerve, which controls the deltoid muscle, may be particularly vulnerable. Many nerve injuries are temporary and improve over weeks to months. Symptoms might include numbness, weakness, or altered sensation. Physical therapy often helps facilitate recovery.
Rotator Cuff Tear
Your rotator cuff muscles help stabilize and move your shoulder after replacement. A tear in these muscles can compromise function and potentially lead to instability. Some patients have rotator cuff damage before surgery that may progress afterward. Others may develop new tears from trauma or overuse.
Stiffness and Limited Range of Motion
Some stiffness is normal early after surgery. However, persistent stiffness limiting daily activities may indicate a problem. Excessive scar tissue, inadequate rehabilitation, or improper positioning can contribute. Working closely with your physical therapist and following your rehabilitation program helps prevent problematic stiffness. Your surgeon may recommend more aggressive therapy or manipulation under anesthesia if stiffness becomes severe.
Prevention and Management Strategies
While you cannot eliminate all risks associated with shoulder replacement, several strategies can help minimize complications and optimize outcomes.
Choosing an Experienced Shoulder Surgeon
Shoulder replacement is a technically complex procedure requiring specialized expertise in shoulder anatomy, biomechanics, and surgical technique. Research consistently demonstrates that surgeon experience significantly impacts patient outcomes.
Studies show that surgeons who perform higher volumes of shoulder replacements achieve lower complication rates, reduced risk of revision surgery, fewer serious adverse events, and shorter hospital stays compared to lower-volume surgeons.
While many factors contribute to successful results, selecting a surgeon with substantial shoulder arthroplasty experience represents an important step in optimizing your outcome. During your consultation, don’t hesitate to ask about your surgeon’s experience with shoulder replacement, annual case volume, and outcomes in patients similar to you.
Pre-operative Preparation
Optimizing your health before surgery sets the foundation for successful recovery. This includes managing chronic conditions if possible. Your surgeon may ask you to stop certain medications temporarily. If you smoke, stopping several weeks before surgery may help reduce complication risks.
Surgical Technology
Advances in surgical techniques and implant technology continue to improve outcomes from shoulder replacement. Computer-assisted planning allows your surgeon to carefully assess your anatomy before entering the operating room. This technology helps optimize implant positioning and sizing for your specific anatomy.
Post-operative Care
Following your surgeon’s instructions is essential. This includes wearing your sling as directed, keeping the incision clean, and attending follow-up appointments. Report any concerning symptoms promptly to your medical team.
Rehabilitation
Physical therapy often plays a role in achieving optimal outcomes. Your therapist will guide you through exercises designed to restore motion, build strength, and improve function. Consistency with your home program is important, as well as attending sessions. Progress typically follows stages. Early exercises focus on gentle motion. As healing progresses, you may advance to strengthening activities.
Long-term Activity Modifications
While modern shoulder replacements are durable, they have limitations. High-impact activities and heavy lifting can place excessive stress on components. Many surgeons recommend avoiding contact sports and heavy overhead lifting. Lower-impact sports may be acceptable with precautions.
When to Contact Your Surgeon
Recognizing potential problems early allows for timely intervention. Contact your surgeon if you experience:
- Increasing pain that doesn’t respond to medication
- Fever, chills, or signs of infection at the surgical site
- Sudden loss of motion or function
- Severe swelling or drainage from the incision
- A feeling that your shoulder is slipping or unstable
- Numbness or weakness that seems to be worsening rather than improving
Don’t hesitate to reach out with concerns, even if you’re unsure whether something is normal. Your surgical team would rather address potential issues early than wait until problems become more serious.
Summary
Total shoulder replacement surgery has helped many patients return to comfortable, active lives after painful shoulder conditions made daily activities challenging. While problems after shoulder replacement surgery can occur, understanding these potential complications can help you make informed decisions and recognize issues early if they develop. Glenoid loosening represents one of the more common long-term concerns with anatomic shoulder replacement, though modern implant designs are working to address this challenge through improved mechanical stability and stress distribution.
An experienced surgical team employs numerous strategies to minimize risks, including careful surgical technique, appropriate implant selection, and comprehensive post-operative care protocols. Your own efforts in preparing for surgery, following post-operative instructions, and committing to rehabilitation may also influence your outcome. Open communication with an experienced shoulder surgeon throughout the process ensures any problems are addressed promptly and effectively.
Frequently Asked Questions
What is glenoid loosening?
Glenoid loosening occurs when the plastic socket component (glenoid) begins to separate from the bone where it was implanted. Over time, the repetitive forces during shoulder movement can create gaps at the bone-cement interface, potentially leading to pain and decreased function.
Can glenoid loosening be prevented?
While glenoid loosening cannot be entirely prevented, several strategies reduce risk. Proper implant positioning is essential. The InSet® Glenoid from Shoulder Innovations is designed to reduce the mechanical stresses associated with glenoid loosening. Following activity guidelines after surgery can help protect long-term stability.
What activities should I avoid after shoulder replacement?
Most surgeons recommend avoiding high-impact activities, contact sports, heavy overhead lifting, and repetitive heavy labor. Activities with falling risk should be approached cautiously. Low-impact activities like swimming, golf, and doubles tennis are generally acceptable. Discuss your specific goals with your surgeon for personalized recommendations.
Is pain normal after shoulder replacement surgery?
Some post-operative pain is normal as your body heals. This should gradually improve over weeks to months. Pain that increases, sudden severe pain, or pain with other symptoms like fever may require evaluation by your surgeon.



