Shoulder pain and dysfunction can interfere with daily life, limiting mobility, disrupting sleep, and hindering participation in activities once enjoyed. For many individuals suffering from severe shoulder arthritis or irreparable damage, total shoulder arthroplasty, commonly known as total shoulder replacement surgery, offers a potential solution. This advanced orthopedic procedure involves replacing damaged bone and cartilage with prosthetic components, with the goal of alleviating pain and restoring a greater range of motion and function to the shoulder joint.
Key Takeaways
- Anatomic total shoulder arthroplasty aims to replicate the natural ball-and-socket structure of the shoulder, replacing both the humeral head (ball) and the glenoid (socket) with prosthetic components.
- Conditions treated primarily include osteoarthritis, rheumatoid arthritis, post-traumatic arthritis, and osteonecrosis of the shoulder.
- The procedure involves a precise surgical technique to remove damaged bone and cartilage, prepare the bone surfaces, and implant the prosthetic components, typically under general anesthesia with a nerve block.
- Recovery is a gradual process, often involving an initial period of immobilization in a sling, followed by a structured physical therapy program to regain strength and mobility. Full recovery can take several months to a year.
Understanding Shoulder Anatomy
The shoulder is one of the most complex and mobile joints in the human body, allowing for an extensive range of motion necessary for countless daily activities. The shoulder is formed by three primary bones: the humerus (the long bone of the upper arm), the scapula (shoulder blade), and the clavicle (collarbone).
At the core of the shoulder’s mobility is the ball-and-socket mechanism. The rounded head of the humerus acts as the “ball,” and a shallow, cup-shaped depression in the scapula called the glenoid serves as the “socket.” Both the humeral head and the glenoid are covered by a slippery tissue called articular cartilage to facilitate smooth movement.
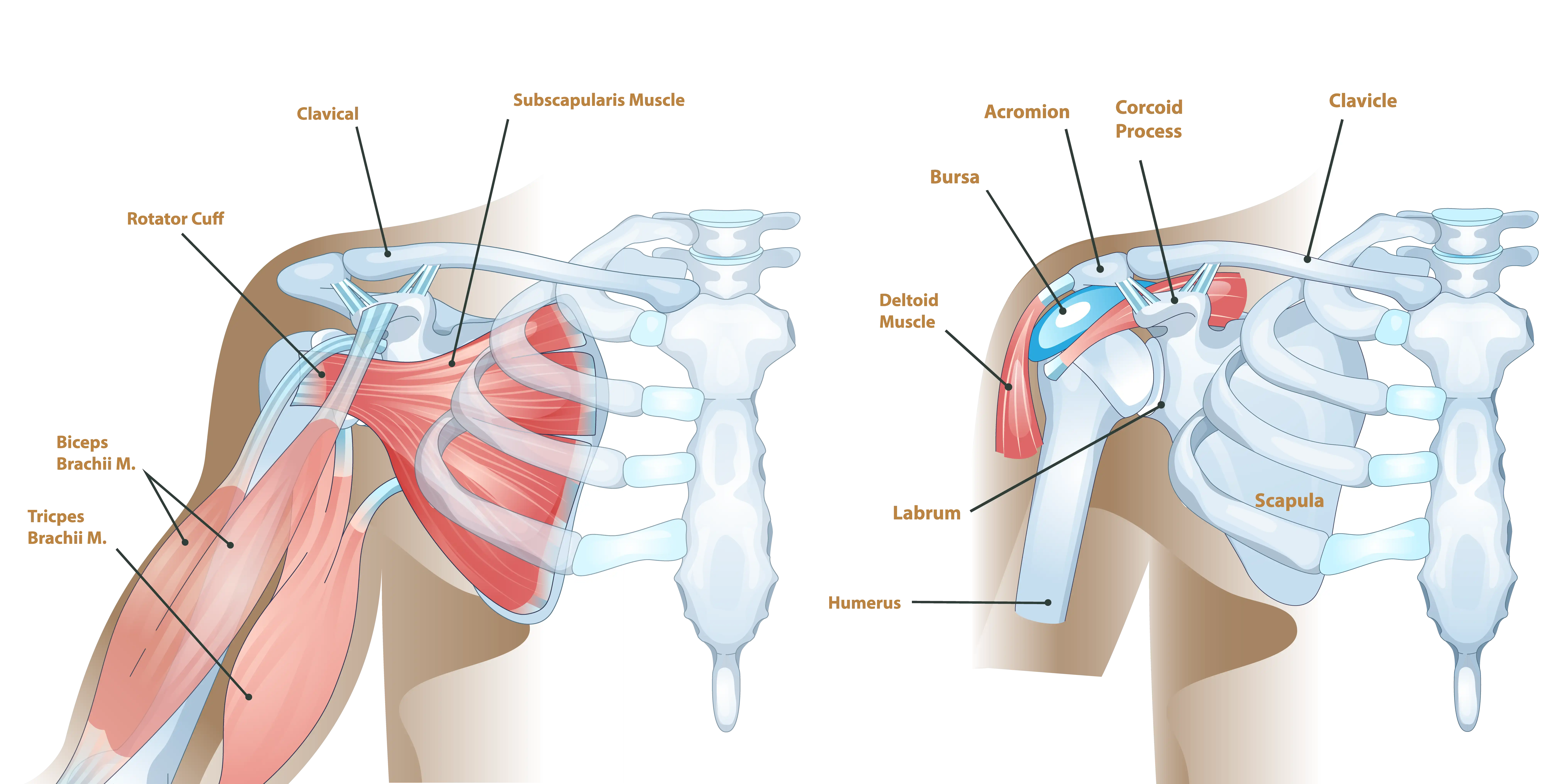
Stabilizing this highly mobile joint is the rotator cuff, a group of four muscles and their tendons that surround the shoulder joint. The rotator cuff also plays a key role in powering shoulder motion. When any of these components become damaged, it can lead to pain, stiffness, and a reduction in the shoulder’s ability to function normally.
Conditions Treated by Anatomic Total Shoulder Replacement
Total shoulder arthroplasty is primarily recommended for individuals experiencing severe shoulder pain and functional limitations due to advanced joint damage that has not responded to conservative treatments. The goal of an anatomic total shoulder replacement is to restore the natural ball-and-socket configuration of the shoulder, closely mimicking its original anatomy. This procedure may be particularly effective for several conditions, which we’ll explore in the following subsections.
Osteoarthritis (Degenerative Joint Disease)
Osteoarthritis, often referred to as “wear-and-tear arthritis,” is the most common reason for total shoulder replacement. Over time, the smooth articular cartilage covering the ends of the humeral head and glenoid gradually wears away. This can lead to bone-on-bone friction, causing pain, stiffness, and a grinding sensation in the joint.
Rheumatoid Arthritis and Other Inflammatory Disorders
Rheumatoid arthritis is an autoimmune disease where the body’s immune system mistakenly attacks its own tissues, including the synovial lining of the joints. This chronic inflammation can lead to significant damage to the articular cartilage and underlying bone in the shoulder joint. Other inflammatory conditions can also cause similar changes.
Post-Traumatic Arthritis
Previous injuries to the shoulder, such as fractures of the humerus or glenoid or dislocations, can accelerate the wear and tear on the joint surfaces. Even after successful treatment of the initial injury, the altered mechanics or damage to the cartilage can lead to the development of post-traumatic arthritis years later, resulting in chronic pain and dysfunction.
Osteonecrosis (Avascular Necrosis)
Osteonecrosis, also known as avascular necrosis, occurs when the blood supply to the humeral head is disrupted. Without adequate blood flow, the bone tissue dies and eventually collapses, leading to severe pain and joint destruction.
The Anatomic Total Shoulder Replacement Procedure
Anatomic total shoulder replacement is a sophisticated surgical procedure performed by an experienced shoulder surgeon, designed to alleviate pain and restore function by replacing the damaged components of the shoulder joint with prosthetic implants. The surgery typically takes 1 to 3 hours and is performed under general anesthesia, often combined with a nerve block to provide extended pain relief post-operatively.
The general steps involved in an anatomic total shoulder replacement procedure include:
- Incision: The surgeon makes an incision, usually along the front of the shoulder (deltopectoral approach), to access the joint.
- Area preparation: The damaged components are carefully removed and the sites are prepared to receive the prosthetic components.
- Prosthetic insertion: The prosthetic components are placed. The size and position of these components are carefully selected to match the patient’s anatomy and restore optimal joint mechanics.
- Closure: After the prosthetic components are securely in place and the joint’s stability and range of motion are confirmed, the soft tissues, including the subscapularis muscle (part of the rotator cuff), are carefully repaired. The incision is then closed.
Recovery Process After Total Shoulder Arthroplasty
The recovery journey following total shoulder arthroplasty is an important phase that often requires patience, commitment, and adherence to a prescribed rehabilitation program. While individual recovery times can vary, we’ll explore a typical timeline, broken into phases.
Immediate Post-Operative Period
Immediately after surgery, most patients will experience some pain and swelling, which may be managed with medication and ice. The arm will be placed in a sling or immobilizer to protect the healing tissues and prevent unwanted movement. Patients may begin gentle passive range-of-motion exercises under the guidance of a physical therapist.
Early Rehabilitation
During this phase, physical therapy sessions may become more regular, focusing on restoring passive and then active range of motion, gradually increasing the intensity of exercises. The goal is to prevent stiffness and promote healing without stressing the surgical repair. Patients are usually advised to avoid lifting, pushing, or pulling with the affected arm. Light daily activities, such as getting dressed and simple chores, can typically be resumed after a few weeks.
Advanced Rehabilitation
As healing progresses, the physical therapy program advances to include strengthening exercises for the rotator cuff and deltoid muscles. The focus shifts from passive motion to active motion and regaining functional strength. Patients gradually increase their activity levels, but heavy lifting and strenuous activities are still restricted. The physical therapist will guide the patient through exercises designed to improve overall shoulder mechanics and prepare them for a return to more demanding activities.
Long-Term Recovery and Return to Activity
Full recovery from total shoulder arthroplasty is a journey that can extend from six months to a full year, and sometimes even longer, depending on individual factors such as age, overall health, the severity of the initial condition, and adherence to the rehabilitation program. Most patients find they can comfortably resume the majority of their normal daily activities, including many recreational sports and hobbies they may have had to abandon due to shoulder pain.
It is important to understand that while the surgical intervention provides the foundation for recovery, the long-term success of total shoulder arthroplasty often relies on consistent adherence to a home exercise program and lifestyle modifications. Regular exercise helps maintain the strength and flexibility gained during physical therapy, while avoiding activities that place excessive stress on the new joint can prolong its lifespan. Your surgeon and physical therapist will provide personalized recommendations regarding activity levels and any necessary precautions to support the longevity of your shoulder replacement and your continued well-being.
Summary
Total shoulder arthroplasty is a surgical procedure that offers significant relief from chronic shoulder pain and improved function for many individuals suffering from advanced shoulder arthritis or other debilitating conditions. By replacing damaged joint surfaces with prosthetic components, patients can often regain the ability to perform daily tasks, enjoy a better quality of life, and return to activities they once loved. Understanding the anatomy of the shoulder, the conditions that may necessitate surgery, the details of the procedure, and the commitment required for rehabilitation are key steps for anyone considering this operation.
Frequently Asked Questions (FAQs)
Will I regain full range of motion after surgery?
Most patients experience significant improvement in their range of motion and a substantial reduction in pain. While complete restoration to pre-injury or pre-arthritic levels may not always be possible, the goal is to achieve a functional range of motion that allows for comfortable participation in daily activities and many recreational pursuits. The extent of motion regained depends on various factors, including the condition of the shoulder before surgery and commitment to physical therapy.
How soon can I return to normal activities, including sports?
Return to activities may be gradual. Light daily activities can often be resumed within a few weeks. More strenuous activities and sports typically require several months of rehabilitation. Your surgeon and physical therapist will provide specific guidance based on your individual progress and the demands of your desired activities.
Is total shoulder replacement very painful?
Pain management is a priority during and after surgery. Patients typically receive general anesthesia and a nerve block to minimize immediate post-operative pain. After surgery, pain may be managed with medication and ice. While some discomfort is expected during the initial recovery and rehabilitation phases, it is generally manageable and improves over time as healing progresses.
What is the difference between anatomic and reverse total shoulder replacement?
In an anatomic total shoulder replacement, the implants mimic the natural anatomy: a ball on the humerus and a socket on the glenoid. This is typically used when the rotator cuff is healthy and functional. In a reverse total shoulder replacement, the ball and socket are reversed: a ball is placed on the glenoid and a socket on the humerus. This design is often preferred for patients with a severely damaged or non-functional rotator cuff, as it relies on the deltoid muscle for arm elevation instead of the rotator cuff.



